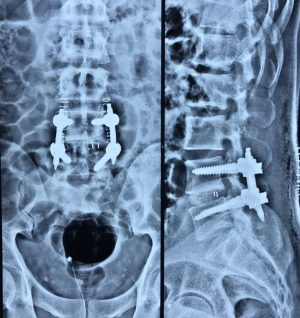
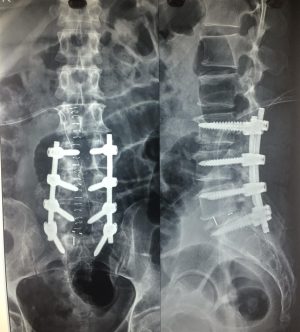
Spinal Fusion Surgery
Spine Fusion and Instrumentation Surgery
Spinal fusion surgery involves joining two or more vertebrae together. This is done to prevent movement between adjacent vertebrae. Spine fusion is usually accompanied by spine instrumentation using various spine implants. It is extremely important to understand difference between spine fusion and spine instrumentation. Fusion is union of one vertebra with another vertebra with the help of bone graft. Spine instrumentation is done to help immobilize the spine until fusion takes place. Fusion will provide long term success to a spine instrumentation surgery. If fusion does not take place, there will be constant stress on spine implant and eventually it will fail (will either become loose in the bone or will break). Spine decompression is usually done along with spine fusion surgeries.
Indications of Spine Fusion Surgery:
- Spine fractures,
- Spine infection/ tuberculosis with significant destruction of vertebra,
- Spine tumors with significant destruction of vertebra,
- Spondylosis causing severe back pain or neck pain,
- Spine deformity correction surgery (scoliosis, kyphosis).
- Spondylolisthesis (especially the one with spondylolysis).
- Severe stenosis requiring excessive bone removal for adequate decompression.
- No prevent spine instability in future.
Types of Spine Fusion Surgery:
Spine can be approached from posterior, anterior or lateral side. Various implants are available for different parts of spine and type of approach used. Sometimes, two or more approaches need to be combined to achieve desired results. Following are commonly done spine fusion surgeries:
- Cervical Spine:
- Atlanto-Axial Fusion
- Anterior Cervical Discectomy/ Corpectomy and Fusion
- Posterior Cervical Lateral Mass Fusion
- Thoracic Spine:
- Posterior Thoracic Fusion
- Anterior (Trans-thoracic) Thoracic Fusion
- Lumbar Spine:
- Posterior Lumbar Fusion: PLF/ PLIF/ TLIF/ MIS TLIF
- Anterior Lumbar Fusion: ALIF
- Lateral Lumbar Fusion: XLIF, OLIF
- Lumbar-Sacral-Iliac Fusion:
- Posterior Lumbo-sacral/ Lumbo-sacro-iliac Fusion
- Anterior L5-S1 fusion: ALIF
- Sacro-iliac (SI) Joint Fusion:
- Posterior SI Joint Fusion
Advantages of Spine Fusion Surgery:
- Prevention of recurrence of spondylosis/ spine stenosis at fused level,
- Correction of spine deformity,
- mechanical support to spine when vertebrae are significantly destroyed (spine infection/ tuberculosis/ tumors).
- elimination of movements in spondylosis to provide pain relief from arthritic spine joints.
- Reduction of spondylolisthesis.
Disadvantages of Spine Fusion:
- Surgery is bigger magnitude than spine decompression alone,
- Fusion causes stiffness at fused levels due to loss of movements,
- Recovery takes slightly longer,
- Cost of the surgery increases due to
- Added cost of implants
- Additional time spent for fusion during surgery
- Additional hospital stay
- Adjacent Segment Degeneration (ASD): Fusion leads to loss of movements at fused vertebrae. This causes increased movements at free levels next to fused vertebrae as body tries to compensate for lost movements at fused levels. This can accelerate degeneration process at these adjacent levels leading to symptoms of spondylosis.
- If fusion does not takes place, implant will not be able to withstand constant stress of vertebral movement. This might lead to eventual loosening or breakage of the implant.
- Implants can be a source of continuous irritation of soft tissues in vicinity and can cause pain.
Contraindication to Spine Instrumentation Surgery:
- Severe Osteoporosis: A spine implant will not hold in osteoporotic bone. Also, bone fusion is slow and compromised in osteoporotic patients.
- Infection: It is advisable to avoid spine instrumentation in the presence of severe bacterial infection. Presence of metallic implant may inhibit infection healing.
- Uncontrolled Diabetes: Patients with high sugar are prone to develop infection. Presence of metallic implants may provide more favorable environment to bacteria to grow and make eradication of infection difficult. Severe Medical Illnesses/
- Immunocompromised/ Poor Nutritional Status: A spine instrumentation surgery is of bigger magnitude and better avoided in patients with associated medical risk. These patients have a higher risk of. Bone healing required with instrumentation procedure is usually compromised in patients.
- Multilevel Procedures: Instrumentation prohibits movement at operated level. A one or two level spine instrumentation will not create any significant change in patient’s mobility. However, a multilevel instrumentation can significantly affect patients mobility, especially in lumbar spine.
For these patients, fusion can be attempted without instrumentation. However, rate of fusion is lower compared to instrumented surgeries. Spine specialists take all the risks and benefits into consideration while deciding whether 1) a fusion surgery is required or only decompression will suffice, 2) if fusion is necessary, whether an instrumentation can be done safely or it is better to avoid instrumentation and try to achieve non-instrumented fusion.
Recent Advances in Spine Fusion Surgeries:
- Minimally Invasive Spine Surgery: With the availability of microscope and specialized retractors most of the routine fusion surgeries can be done in a minimally invasive fashion. This provides all advantages of a minimally invasive surgery.
- Percutaneous Pedicle Screws: Pedicle screws are most commonly used lumbar implants. Traditional lumbar surgeries involve lot of muscle dissection to insert pedicle screws. Percutaneous pedicle screw systems allow insertion of pedicle screws through tiny holes in skin causing minimum muscle damage and bleeding.
- Computer Navigation and Robot Guided Spine Surgery: A preoperative CT scan or intra-operative fluoroscopy images are fed in a computer. Specialized navigations tools are then used to help spine surgeons pass pedicle screws. This technology is especially useful for minimally invasive spine surgeries, instrumentation of severely deformed bones and in revision surgeries where routine bony landmarks are not available to guide surgeon to pass pedicle screws.