Lumbar Interbody Fusion
Lumbar Spine Fusion Surgery
Lumbar interbody fusion involves complete discectomy and inserting a cage with bone graft between two vertebral bodies. A fusion done in the interbody area has most favorable chance to succeed due to wider surface area and ability to accommodate large amount of graft.
Types of Lumbar Interbody Fusion:
- Posterior Lumbar Interbody Fusion (PLIF): A posterior approach is used to access interbody area. Space between spinal cord and facet joint is used to enter disc and do interbody job. This is traditional method of lumbar interbody fusion.
- Trans-Foraminal Lumbar Interbody Fusion (TLIF): A posterior approach is used similar to PLIF; however, interbody area is accessed by resecting the bone lateral to spinal cord. This avoids excessive retraction of spinal cord to avoid nerve irritation. TLIF is especially useful in revision surgeries to avoid scar tissue around spinal cord from previous surgery. This approach is also used for minimally invasive lumbar interbody fusion (MIS TLIF).
- Anterior lumbar Interbody Fusion (ALIF): Lumbar intervertebral disc is accessed from an anterior (trans-abdominal) approach. Advantage of this procedure is that a very big cage can be inserted. A bigger cage supports lumbar vertebrae better and allow more bone graft insertion for fusion.
- Lateral/ Extreme Lateral Lumbar Interbody Fusion (LLIF/ XLIF): Interbody area is accessed by a lateral approach. A cage is inserted in left-right direction spanning the entire width of the disc space. LLIF provides robust support to lumbar vertebrae and accommodates large quantity of graft for fusion. LLIF can be done in a minimally invasive way. They are commonly used for correction of adult degenerative scoliosis deformities.
- Oblique Lumbar Interbody Fusion (OLIF): OLIF is similar to LLIF other than that disc is entered slightly anteriorly. This prevents psoas muscle disruption, which is a common cause of thigh soreness after LLIF surgery.
Occasionally, lumbar spine is fused without interbody cage/ grafting. This is called posterolateral Lumbar fusion (PLF) wherein fusion is attempted at facet joint or nearby outer aspect of vertebra. All fusion techniques have one common purpose, achieving union between two vertebral bodies. These approaches are used in different situation as per the unique requirement of the case and surgeon’s preference.
One lumbar fusion technique deserves special mention:
- MIS TLIF (Minimally Invasive Trans-Foraminal Lumbar Interbody Fusion): MIS TLIF is most commonly performed lumbar fusion surgery. It combines concepts of minimally invasive lumbar decompression and minimally invasive lumbar fusion surgery. Specialized tubular or expandable retractors are used to perform lumbar decompression and interbody fusion (TLIF), using cage spacer and bone graft. Pedicle screws are then placed 1) through expandable retractors, 2) percutaneously using fluoroscopy, 3) using computer navigation/ robotics.
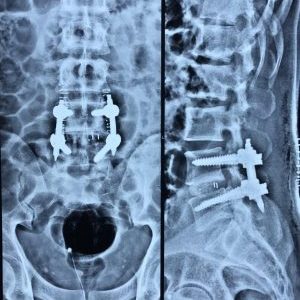
MIS TLIF Surgery
Spinal fusion is a highly effective surgical procedure used to treat various spinal conditions, providing stability and relief to countless individuals. However, like any surgery, it comes with its unique set of challenges during the recovery period. In this article, we will explore some common problems that patients may encounter after spinal fusion surgery and offer guidance on how to manage them.
1. Postoperative Pain:
– It’s common to experience pain at the surgical site immediately after spinal fusion surgery. Your surgeon will prescribe pain medications to help manage this discomfort. It’s essential to take these medications as directed and communicate any issues with pain management to your healthcare team.
2. Limited Mobility:
– Following spinal fusion, patients often experience limited mobility due to the surgical site’s immobilization and the need to protect the newly fused spine. Your surgeon will provide guidelines on movement restrictions. Physical therapy and exercises tailored to your condition can aid in gradually regaining mobility over time.
3. Nerve Irritation:
– In some cases, nerve irritation or inflammation may occur after spinal fusion surgery. This can lead to symptoms such as tingling, numbness, or weakness in the legs or arms. It’s essential to report any new or worsening neurological symptoms to your surgeon promptly.
4. Infection Risk:
– While infection after spinal fusion is relatively rare, it’s a potential complication. Patients should closely monitor the surgical site for signs of infection, such as increased redness, swelling, warmth, or unusual discharge. If any of these symptoms occur, contact your surgeon immediately.
5. Fusion Failure:
– Although spinal fusion has a high success rate, there is a possibility of fusion failure, where the vertebrae do not fully fuse together. Smoking and poor nutrition can increase the risk of fusion failure. Compliance with post-operative instructions, including activity restrictions and a balanced diet, is crucial to enhance fusion success.
6. Hardware Issues:
– In some cases, hardware such as screws or rods used during the fusion procedure may cause discomfort or complications. This can include hardware migration or irritation. If you experience unusual pain or discomfort around the surgical site, it’s essential to discuss these concerns with your surgeon.
7. Psychological Impact:
– The recovery period following spinal fusion surgery can be mentally challenging. Patients may experience anxiety, depression, or frustration due to limitations in mobility and daily activities. Seeking emotional support from loved ones or professional counseling can help navigate these emotional challenges.
8. Medication Side Effects:
– Some patients may experience side effects from post-operative medications, such as nausea, constipation, or drowsiness. If you encounter these issues, communicate with your healthcare team to explore alternative medications or strategies for managing side effects.
In conclusion, understanding and addressing common problems after spinal fusion surgery is crucial for a successful recovery. Effective pain management, close monitoring for signs of complications, adherence to post-operative guidelines, and open communication with your healthcare team are key factors in ensuring a smoother recovery journey.
It’s important to note that each patient’s experience may vary, and some individuals may encounter fewer or different challenges during their recovery. Your surgeon and healthcare team are your greatest allies in managing these issues, so do not hesitate to reach out to them with any concerns or questions. With proper care and attention, the majority of patients can achieve improved spinal health and a better quality of life after spinal fusion surgery
Spinal fusion surgery is a remarkable procedure that can provide much-needed relief from debilitating spinal conditions. However, like any surgical intervention, it may come with certain limitations and permanent restrictions. In this article, we will explore what patients can expect in terms of permanent restrictions after spinal fusion surgery and how to navigate life with these limitations.
1. Physical Activity Limitations:
– One of the most significant permanent restrictions after spinal fusion is a limitation on certain physical activities. Your surgeon will provide specific guidelines on activities to avoid or modify to protect the fused spine. Common restrictions may include heavy lifting, twisting, or strenuous bending.
2. Reduced Spinal Mobility:
– Spinal fusion aims to stabilize the spine by fusing two or more vertebrae together. While this enhances spinal stability, it may reduce the mobility of the fused segment. The degree of reduced mobility depends on the number of vertebrae fused and the location of the fusion.
3. Impact on Range of Motion:
– Patients who undergo spinal fusion in the lumbar (lower back) region may experience a reduction in their range of motion when bending forward or backward. This can affect activities like bending to tie shoelaces or reaching for objects on the ground.
4. Restrictions on Work and Daily Activities:
– Depending on your occupation and the nature of your daily activities, you may need to make adjustments or accommodations to accommodate the permanent restrictions. Jobs that require heavy lifting or repetitive bending may be challenging to maintain.
5. Impact on Sports and Exercise:
– Engaging in certain sports or exercise activities may become more challenging after spinal fusion. High-impact sports and activities that involve twisting or sudden, vigorous movements may be discouraged. However, many individuals can still enjoy low-impact exercises like swimming, walking, or cycling.
6. Lifestyle Modifications:
– Adapting to permanent restrictions after spinal fusion may require lifestyle modifications. Simple changes, such as using assistive devices for reaching high shelves or avoiding heavy lifting, can help you maintain independence and minimize strain on your spine.
7. Psychological Adjustment:
– Coming to terms with permanent restrictions can be emotionally challenging. It’s essential to acknowledge any feelings of frustration, sadness, or disappointment and seek support from loved ones or a mental health professional if needed. Maintaining a positive outlook and focusing on what you can do rather than what you can’t can help improve your quality of life.
8. Regular Follow-Up Care:
– To ensure the success of your spinal fusion and to monitor any potential complications or changes in your condition, it’s crucial to continue with regular follow-up appointments with your surgeon. These appointments allow your surgeon to assess your progress, provide guidance, and address any concerns.
It’s important to note that the specific permanent restrictions after spinal fusion can vary depending on factors such as the location and extent of the fusion and the individual patient’s condition. Your surgeon will provide you with personalized guidance on what to expect and how to adapt to these limitations.
While permanent restrictions may pose challenges, many individuals successfully navigate life after spinal fusion by making necessary adjustments and focusing on their overall well-being. Remember that the goal of spinal fusion surgery is to improve your spinal health and quality of life, and with proper care and support, you can lead a fulfilling and active life within the scope of these restrictions.

very good illustration of lumbar spine fusion
Thank you Dr. Atmaram.