Posterior Cervical Spine Surgery
Cervical Spine Fusion Surgery
A cervical laminectomy/ posterior cervical decompression surgery is required for various conditions. Posterior cervical decompression can be combined with fusion and instrumentation if required.
Indications for Posterior Cervical Surgery:
- Cervical Myelopathy with multilevel cervical spinal cord compression: A multilevel Cervical laminectomy is a far easier and faster procedure compared to multilevel anterior cervical decompression and fusion.
- Less morbid for patients with associated medical problems,
- Avoids multilevel fusion required with anterior procedure,
- A decompression (laminectomy/ Laminoplasty) alone can be done without fusion/ instrumentation in selected cases,
- Posterior Compression: Presence of a posterior compression (with/ without associated anterior compression) usually requires posterior decompression procedures.
- Severe Cervical Instability: Patients with cervical spine fracture, spine infection and spinal tumors, might require additional posterior spinal instrumentation/ fusion addition to an anterior decompression and fusion procedure.
Sometimes, a combined anterior and posterior cervical spine surgery is required depending upon the nature of the pathology. These both surgeries can be done at the same time or can be staged with few days difference between both surgeries.
Advantages of Posterior Cervical Surgery:
- Relatively simple procedure compared to anterior cervical surgery,
- Able to tackle multi-level pathology easily,
Disadvantages/ Limitations of Posterior Cervical Surgery:
- Can cause cervical kyphosis due to loss of posterior stabilizing factors (if not instrumented/ fused),
- Incidence of neck pain is higher in patients after posterior cervical surgery,
- An anterior procedure may be required after posterior surgery if there is persistent anterior spinal cord compression causing symptoms.
Type of Posterior Cervical Surgery:
- Cervical Laminectomy: Posterior arch of the cervical vertebra (lamina) is removed at compressed levels.
- Cervical Laminectomy and Fusion: In addition to cervical laminectomy, a lateral mass or pedicle screw instrumentation is done to achieve fusion at operated levels. This is required to prevent post-operative cervical kyphosis and recurrence of symptoms.
- Cervical Laminoplasty: In this procedure, cervical spinal canal is widened by opening the laminae by creating a door mechanism. lifting the laminae off the spinal cord. Laminae are still attached to native vertebrae. A fusion is not performed between different vertebrae. This procedure has following advantages:
- Reduced neck pain (as happens in cervical laminectomy),
- No loss of motion as fusion is not attempted (vis a vis posterior cervical fusion),
- Preserves stability to avoid post-op kyphosis and instability without fusion.
Cervical laminoplasty is a technically more demanding procedure. Decompression achieved with this technique is less than a complete cervical laminectomy which may not be adequate in certain cases. Preservation of motion may not be as desired as auto-fusion occurs sometimes between operated levels.
- Posterior Cervical Microforaminotomy: Prolapsed part of cervical disc can be removed from posterior approach using an endoscope or a microscope. This is similar to lumbar discectomy. Unlike anterior cervical discectomy, posterior cervical microforaminotomy does not require fusion and hence preserves motion at operated level.
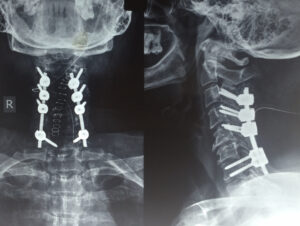
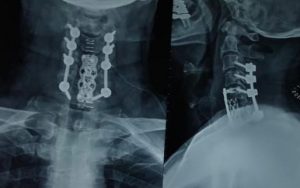
Posterior cervical fusion surgery is a spinal procedure performed on the neck’s posterior (back) side to stabilize and fuse two or more cervical vertebrae together. It is typically done to treat conditions like instability, fractures, or severe degeneration in the cervical spine.
This surgery is recommended when conservative treatments like physical therapy or medication fail to alleviate neck pain, instability, or neurological symptoms caused by cervical spine issues. Common indications include cervical disc herniation, cervical spondylosis, and fractures.
The primary goals are to stabilize the spine, reduce pain, and potentially improve neurological function. The procedure aims to create a solid fusion between the affected vertebrae, preventing further movement.
During the procedure, the surgeon accesses the cervical spine from the back of the neck, removes damaged discs or bone, and inserts bone graft material to facilitate fusion. Metal plates, screws, or rods may be used to provide stability during the healing process.
Yes, minimally invasive techniques may be used in some cases, which involve smaller incisions and potentially shorter recovery times. However, the specific approach depends on the patient’s condition and the surgeon’s expertise.
Recovery time varies but usually involves a few weeks of reduced activity, followed by a gradual return to normal activities. Complete fusion and symptom relief may take several months.
As with any surgical procedure, there are risks, including infection, bleeding, and nerve injury. Your surgeon will discuss potential complications and steps to minimize them before the surgery.
It can be used to correct certain neck deformities or cervical spine alignment issues, but the decision depends on the specific diagnosis and surgical evaluation.
You may need to wear a cervical collar for support initially. Physical therapy may also be recommended to help regain strength and range of motion in the neck.
Look for a spine surgeon with expertise in posterior cervical fusion and a track record of successful outcomes. Consider factors such as experience, patient reviews, and hospital affiliations.
Some post-operative discomfort is common but should improve with time. Your surgeon will provide pain management strategies, which may include medication.
It depends on your insurance plan and the medical necessity of the surgery. It’s advisable to check with your insurance provider before the procedure.
