Best Spine Surgeon in Mumbai | Dr. Amit Sharma

+91-9967600461
draks777@gmail.com
Spinal Stenosis
Spinal Stenosis: Diagnosis and Treatment
Spinal Stenosis Meaning:
Spinal stenosis is a condition in which the spinal canal, which carries the spinal cord and spinal nerves, get narrowed. This causes various symptoms due to pressure on nerve tissue. Some patients have a narrow spinal canal since birth, which becomes symptomatic later on with minimal further stenosis caused by degeneration. This condition is called Congenital/ Developmental Spinal Canal Stenosis. However, in majority of the patients, spinal stenosis is the result of chronic degeneration of tissues in and around the spinal canal.
A herniated disc, arthritic facet joints, and hypertrophied ligamentum flavum contribute in narrowing the spinal canal. Also, as disc height reduces due to progressive degeneration, the openings on the side, called neural foramen, gets constricted leading to pressure on exiting spinal nerves (foraminal stenosis). Similar to a disc herniation, poor posture, heavy laborious activities, obesity, injury to spine can all contribute to early degeneration of the spinal tissues causing spinal stenosis. Spinal stenosis can also be secondary to other major pathologies of the spine, e.g. spinal tumors, spinal infections, spinal tuberculosis, spondylolisthesis, spinal fractures etc.
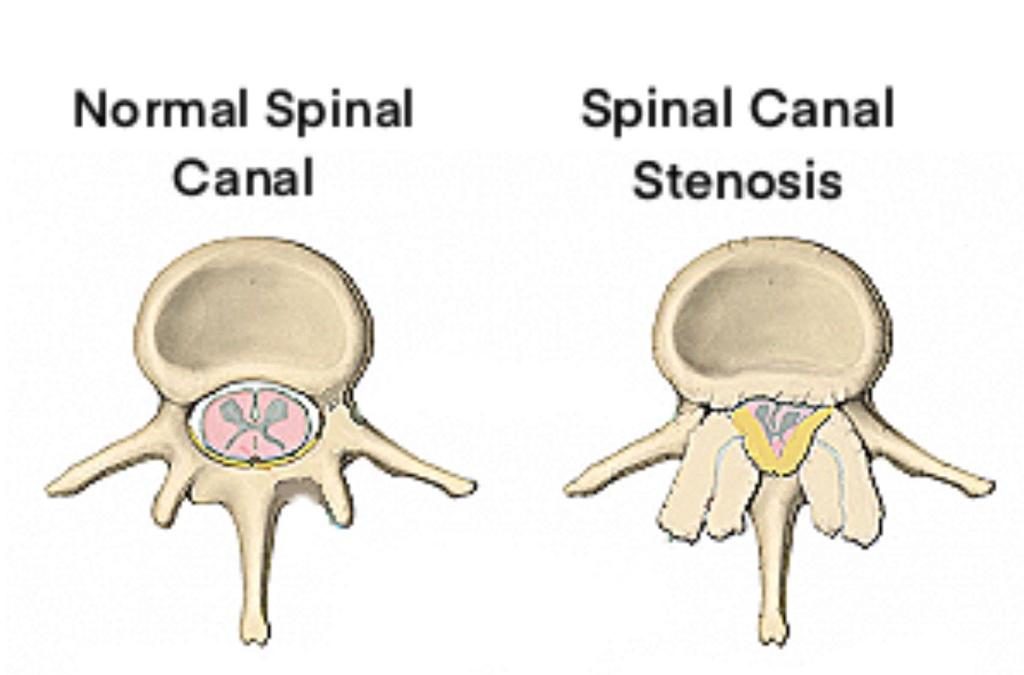
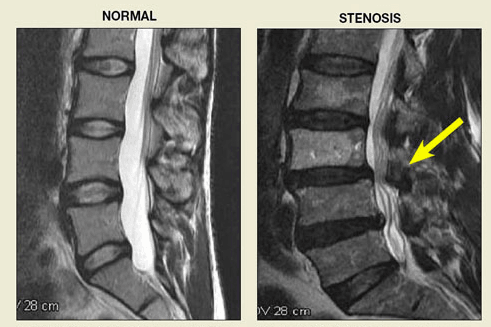
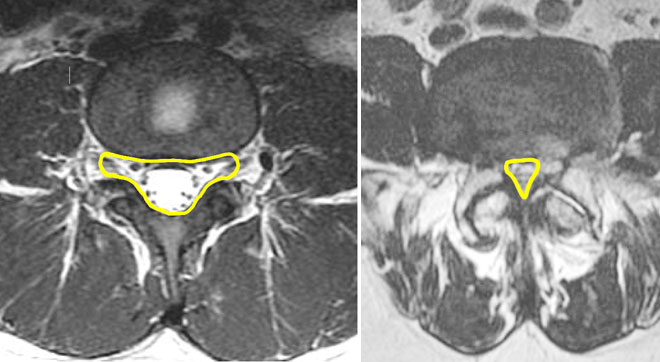
Spinal Stenosis Symptoms:
In Lumbar Spinal Stenosis, patients usually have walking problem, wherein patient is comfortable in resting and sitting position; however, after walking a particular distance, they feel neurological symptoms in legs (Neurological Claudication) in the form of pain, tingling numbness, loss of sensation and weakness in legs. This can sometimes mimic symptoms from loss of blood supply to legs (Vascular Claudication). Though a careful history, physical examination and certain tests can differentiate one from the other. Spinal stenosis in thoracic spine might cause all the symptoms of lumbar canal stenosis with additional loss of balance and spasticity in both legs (Thoracic Myelopathy).
A Cervical Spinal Stenosis will cause symptoms primarily in upper limbs. Along with typical symptoms of nerve pressure, patient will also experience loss of dexterity of hand functions and weakness of hand grip. Also, there will be significant spasticity in upper and lower extremities in severe cases (Cervical Myelopathy). Bladder-bowel can get affected in spinal stenosis at any level indicating severe dysfunction of spinal cord. Recovery in these advance cases is usually slow and incomplete, even after surgical intervention.
Spinal Stenosis Diagnosis:
- History and physical examination,
- MRI Scan: Main diagnostic tool which will show level and severity of pressure on spinal cord,
- X-rays: to rule out bone abnormalities,
- CT Scan: A CT might be required to assess bone structure in detail. Also, C is recommended when MRI cannot be done (patients with heart pacemaker, ear cochlear implants, certain stainless steel orthopaedic implants),
- EMG-NCV: In cases where there is mismatch between MRI picture and patients symptoms. Also when other nerve related abnormalities need to be ruled out, e.g. diabetes, carpal tunnel syndrome, primary neuropathies and myopathies,
- Doppler test: To rule out vascular claudication.
- Blood Tests: Various blood tests might be required to rule out vitamin deficiency (B12), infection, and tumors.
- Other tests: Specific tests to confirm/ rule out infection and tumors might be required, if these conditions are suspected (CT guided biopsy, Histopathology, Culture and Sensitivity etc.)
Spinal Stenosis Treatment:
Spinal stenosis is an irreversible pathology. However, patients symptoms may not correlate with degree of stenosis. Some patients have minimal symptoms even with severe spinal stenosis and others are severely symptomatic even with mild stenosis. Treatment for spinal stenosis is usually based on severity of patients symptoms and response to given treatment.
Medical treatment
: An initial course of pain killer medicines along with local application of pain relieving ointments are used to soothe pain. Other medications are given to make nerve more resistant to painful stimuli to reduce nerve related symptoms (radiculopathy, tingling, numbness). A spinal brace is given to eliminate excessive motion at painful spinal segment and to provide support to spine. Some amount of activity restriction is advisable to prevent worsening of symptoms. Spinal stenosis exercises (physiotherapy) helps in strengthening the back/ neck muscles and reduces muscle spasm.
Epidural Injection
: Similar to disc herniation, epidural injection can be tried in patients with spinal stenosis also for symptomatic relief. A small amount of anaesthetic medication and steroid are injected next to the spinal cord to reduce inflammation. This reduces nerve related symptoms. Epidural injection doesn’t reverse spinal stenosis and help patient buy time before they decide for a definitive treatment. Usually patients get about 4-6 months of significant pain relief; however this might last shorter or longer also. If symptoms recur, injection can be repeated 2-3 times. Epidural injections cannot be given to patients with uncontrolled diabetes and patients on blood-thinner therapy for heart conditions.
Spinal stenosis surgery
: Patients who have severe symptoms to start with or those who don’t respond to above treatment with significant restriction of their day to day activities, usually need removal of pressure from spinal cord. This can be done in various ways-
- Micro-Lumbar Decompression: A Minimally Invasive Spine Surgery using a microscope is usually sufficient for majority of the patient. MIS spine surgery has the advantage of minimal post-operative pain, early hospital discharge and faster recovery.
- Endoscopic Spine Surgery: In selected cases, an endoscopic spinal canal decompression can be done. Some of these cases can be done under local anaesthesia also, which is useful for older patient with multiple medical problems where a full anaesthesia can cause side effects.
- Laminectomy: In patients with severe spinal stenosis, developmental stenosis and multi-level pathology, a formal laminectomy might be the best solution for relief of current symptoms and prevention of recurrence.
In patients with associated significant back pain/ neck pain, severe disc degeneration (spondylosis), slip of vertebra over other (spondylolisthesis), spine fracture (spondylolysis) and spine deformity (scoliosis/ kyphosis), a spine fusion/ instrumentation might also be advised by your spine doctor along with the removal of slipped disc.
If you feel you are suffering from spinal stenosis, please contact Dr. Amit Sharma:
FAQs
Lumbar spinal stenosis usually affect people over 50 years of age. Spinal stenosis is result of a combination of arthritic facet joints between vertebrae, bulging disc and overgrown ligamentum flavum. Primary symptoms of spinal stenosis are leg pain, tingling-numbness in legs, and difficulty in walking and standing. Many patients feel inability to walk long distances (claudication) and they have to sit at regular intervals in between to relieve symptoms. In advance stages there may be loss of sensation and weakness in legs. There may be some amount of back pain associated.
Spinal stenosis is usually a non-reversible condition; however, patient may go through waxing and waning symptoms. Many patients are able to do necessary adjustment in their life style and daily activities to control and avoid progression of spinal stenosis symptoms. Along with anti-inflammatory and nerve medications, certain exercises and precautions can make living with spinal stenosis easier.
A severe spinal stenosis is in which there is severe difficulty in walking with loss of sensation and weakness in legs. MRI usually shows severe compression of spinal cord in these patients. Majority of these patients end up requiring lumbar spinal decompression surgery.
Anti-inflammatory medications are usually required to get pain relief and to reduce inflammation around the nerves. If vitamin B12 is deficient, supplements should be taken. Several nerve stabilizer medications (gabapentin, pregabalin, amitriptyline etc.) are usually taken for long time for symptomatic relief. These medicines makes nerves more resistant against pain and numbness/ tingling.
Spinal stenosis is a permanent condition. A bulging disc might rarely shrink to some extent which might lead to slight reduction in amount of stenosis. However, in old age, disc herniations are usually hard. Also, facetal arthritis and ligamentum flavum hypertrophy are irreversible changes. Severity of spinal stenosis usually progresses with age.
Spinal stenosis symptoms usually worsens with heavy activities. Certain activities (sitting on floor, lifting heavy weights, vigorous exercises) can damage the spine further leading to worsening of spinal stenosis and symptoms.
Various exercises can help patients suffering from spinal stenosis. These exercises helps in various ways
- They help strengthen back muscles and support spine in a better way
- Back exercises help relieve muscle spasms, which will reduce back pain.
- Back exercises load spinal vertebrae, thus making them stronger.
- Exercises maintains flexibility and increase blood flow to intervertebral disc, spin al muscles and other structures of spine to keep them healthy.
- Exercise improves mental and emotional health, and helps in reducing body weight.
Best exercise for spinal stenosis is the one which keeps spine flexible and strong without putting too much pressure on spine. Swimming is one of the best exercise for spine. Bicycle riding, brisk walk and light jogging also can be done as long as it does not worsens your symptoms. It is better to avoid heavy exercises, e.g. weight lifting, vigorous jogging etc., as they may worsen spinal problem.
Surgery is required in severe cases of spinal stenosis where medical treatment is not able to give sufficient relief to the patient. Primarily it’s the patient who has to decide whether his/ her daily life is affected significantly to justify the surgery. In cases with loss of sensation or weakness in legs, surgery is usually needed on urgent basis to preserve and restore nerve functions. If you feel you have tried more than 3 months of medical treatment along with physiotherapy exercises and your symptoms are not improving or worsening, then you should consult your spine doctor to discuss whether a surgery for spinal stenosis will help you.
Spinal stenosis is compression of spinal cord and spinal nerves. Surgery for spinal stenosis involves releasing the pressure from spinal cord. There are several techniques to decompress spinal cord, which is dependent on type of spinal stenosis, severity of spinal stenosis, surgeons’ preference. A minimally invasive technique, e.g. microscopic or endoscopic spine decompression is usually sufficient if your pathology is not very severe. However, for severe pathologies with delayed treatment, a more extensive procedure, e.g. lumbar laminectomy and spinal fusion, might be required. Speak to your spine doctor to understand different options available and best suited procedure for your problem.
Spine surgeries are ever evolving. Newer techniques and technologies are making spine surgeries safer and more effective. Majority of the spinal stenosis surgeries can now be done using Minimally Invasive Spine Surgery techniques. Microscopic tubular spinal decompression and endoscopic spine surgery are primarily used for this purpose. Minimally invasive techniques can also be used for spinal instrumentation and fusion, if required.
My father is suffering neck pain issue and as per MRI found degenerative changes in unconvertabral joints. And age is 67 years. Is any possibility on the said.
Sorry to reply back to you so late. As you are aware, we have already diagnosed him and he is admitted for further care.
Thank you for placing your trust in me.